What Kinds of Treatments are not Covered in Group Health Insurance Plans
Group health insurance is generally offered by employers to their employees. The health insurance indemnifies the policyholders financially in case of hospitalization or injury. The employees may show their group health insurance card in the listed hospital in order obtain treatment from the doctors. However, like every insurance policy, group health insurance too includes certain exclusions. There are some treatments that are not covered in group health insurance policy.
Whom do you want to insure?
- Wallet-friendly plans
- 24/7 claim support
- IRDAI-certified advisors
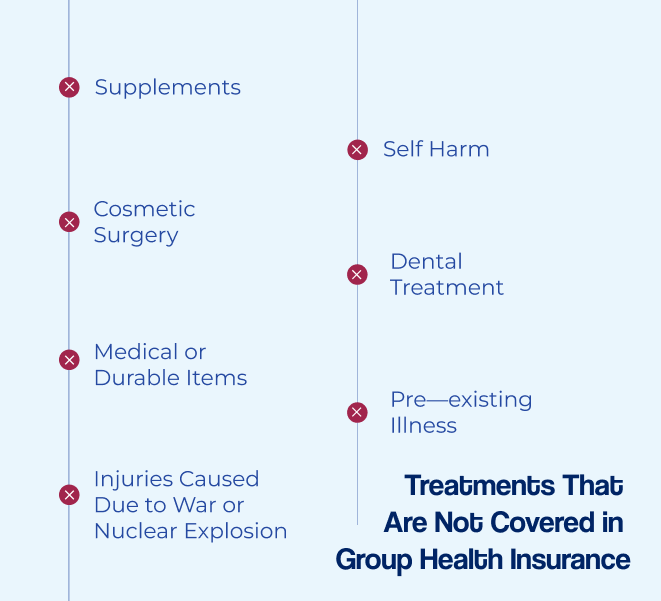
Treatments That are not covered in Group Health Insurance
-
Pre-existing Illness
Pre-existing illness is not precisely an exclusion. The insurer generally does not cover such illness immediately after entering into the insurance deed. Moreover, individual health insurance includes a waiting period of 24 to 48 months for such diseases. However, group health insurance does not include such a period. It may cover the pre-existing disease from day one of the policy. It is also considered as an advantage over individual health insurance.
-
Injuries Caused Due to War or Nuclear Explosion
Whether it is group health insurance or individual health insurance, no one is applicable for any bodily injury caused due to war. Such injuries are excluded from the purview of policy coverage. These are thetreatments that are not covered in group health insurancepolicies. In addition, an injury caused due to a nuclear explosion or radiation shall undeniably be excluded from the coverage of the group health insurance. No insurance covers any loss or damage caused due to war or nuclear explosions. These are the events which are beyond the imagination.
-
Medical or Durable Items
A patient post-treatment may feel the requirement for spectacles, lenses, wheelchairs or lenses. These are essential items for regular and long-term use. The insured may not survive well with these items. However, an individual or policyholder cannot claim such items from the insurance provider. The expenses incurred on such equipment shall extensively be paid by the policyholder. In addition, even if the doctors prescribed such equipment for the patient, the insurance company owns the exclusive right to deny any claim.
-
Supplements
Protein shakes and tonics are not generally consumed by individuals in order to counter any disease. Hence, these are thetreatments that are not covered in group health insurance. However, in case doctors recommend or prescribe the individual to consume such products while the patient is hospitalized, the insurance company is compelled to cover it under thegroup mediclaim policy.
-
Cosmetic Surgery
People need cosmetic surgery to enhance their appearance. It helps them to look fair. However, group health insurance does not cover such treatment. Cosmetic surgery is one of such treatments that are not covered in group health insurance. However, in case of an injury where the doctor suggests plastic surgery, the insurance company is obliged to cover it under group mediclaim policy.
-
Self Harm
Any harm or injuries inflicted by the policyholder to his body shall not cover under the group health insurance plan. The harm or injury must be accidental in nature. If it is found to be self-inflicted, the insurance company owns the full right to exclude such treatment and deny or refuse the claim. Further, this exclusion is explicitly written or mentioned by the insurance company on the insurance brochure and insurance deed.
-
Dental Treatment
Dental treatment is not covered under the group health insurance plan. However, such treatment might be covered if any dental injury arises from an accident.
Conclusion
Group health insurance is provided by the employer to the employees. However, it is not necessary that this policy shall cover every treatment. Pregnancy and pre-existing diseases are some treatments that are not covered under the group health insurance plans. In addition, the group health plan does not provide any coverage for addiction treatments. However, it is important to note that every insurance plan has its own list of exclusions. Therefore, the policyholder or the employer must learn about these exclusions before purchasing such plans.

Group Health Insurance Premium Calculator
Who do you want to insure?
- Employees
- Employees & their family
Minimum lives should be 7
Include maternity coverage
Wellness At Work
Benefits of group health insurance
insurance coverage. Be assured, all your questions
will be answered
Disclaimers+




 Expert advice made easy
Expert advice made easy